CARL. Therapy
CARL Therapy is a new method of resuscitation following cardio-circulatory arrest (“sudden death”), which was developed in an interdisciplinary collaboration of physicians and perfusionists at the Department of Cardiovascular Surgery at Freiburg University Hospital. The innovative approach addresses the frequent occurrence of sudden death which is treatable to a very limited extent so far, even under optimal conditions.
When the heart stops beating.
The human organism depends on a continuous blood flow as blood supplies all cells, tissues and organs with essential nutrients and ensures the removal of metabolic products. If the heart stops, this circulation is interrupted (ischemia) and the energy balance of the cells and organs is impaired within seconds. Subsequently, ischemic damage triggers a series of metabolic adaptations in the cells.
Back on track.
In this situation the pre-damaged organism of an affected patient meets the efforts of first responders and later rescue personnel trying to restore circulation (reperfusion) and to provide oxygen as quickly as possible. This is part of routine cardio-pulmonary-resuscitation (CPR) which includes initially cardiac massage and lay respiratory support (mouth-to-mouth or mouth-to-nose).
Within the framework of an advanced CPR performed by medical staff, the patient is intubated, defibrillated and supplied with appropriate medication. By these means, cardiopulmonary circulation can ideally be restored, and the patient may be transferred to a hospital where the cause of the cardiac arrest can be treated.
Controlled Automated Reperfusion
of the Whole Body.
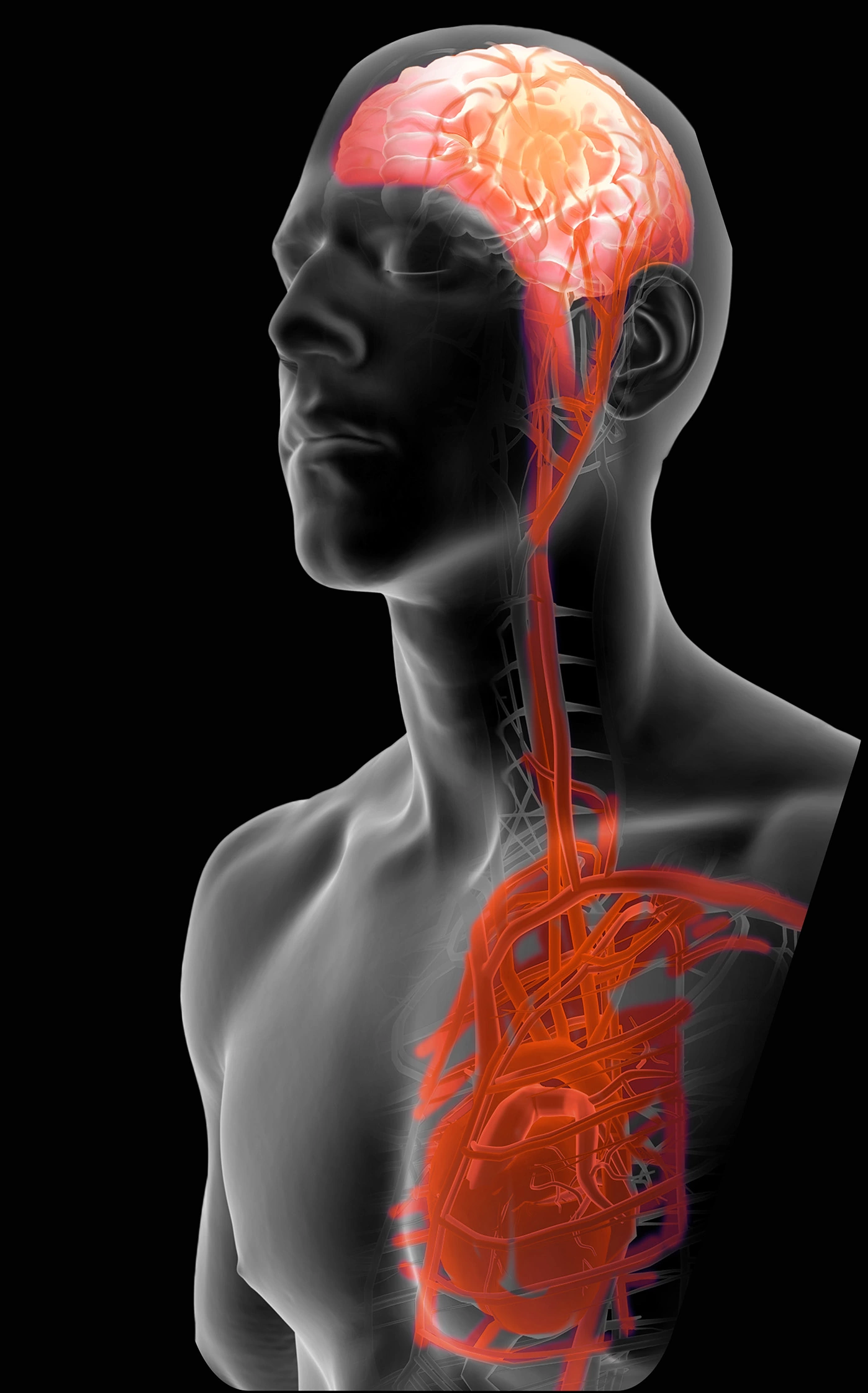
Race against time.
However, the chances of successful resuscitation without neurological sequelae are low as the methods established to date are limited in regard to therapeutical possibilities. Only about ten per cent of all patients survive cardiovascular arrest outside a hospital, afterwards often suffering severe long-term neurological damage. Above all, the brain reacts extremely sensitive to interrupted circulation – but according to recent findings, this refers less to the consequences of ischemia than to the consequences of an uncontrolled resumption of blood flow.
The injurious impact in the phase of reperfusion is, among other things, due to the unspecific supply of oxygen, which cannot be adequately metabolized in the cells pre-damaged by ischemia. Thus, the highly reactive oxygen (free radicals) triggers severe damage to membranes, organelles, protein complexes and other cell components. We therefore refer to the overall damage after cardiac arrest as an ‘ischemia reperfusion injury’.

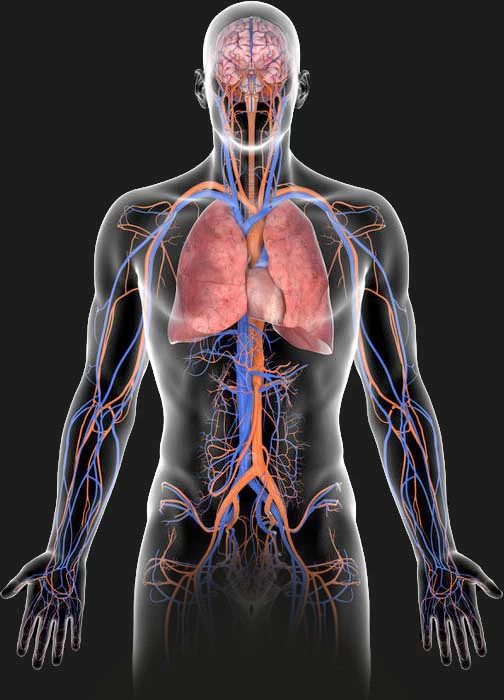
Step-by-step resuscitation.
Within the framework of CARL Therapy, the above pathophysiological changes are taken into account and treated in a targeted manner. To this end, the body’s own circulatory system is first bridged with the aid of two blood pumps and a special tubing system (perfusion set), which is connected to the patient’s circulation via the groin vessels.
Then, important vital parameters – such as the oxygen content and pH value of the blood – are continuously measured and patient-individually modified so that the cells and therefore the whole organism can gradually recover from ischemia and re-establish physiological metabolic processes.
Physical reperfusion conditions, i.e., blood flow, blood pressure and body temperature, are also monitored and specifically adapted. The body core temperature is reduced to about 34 °C right at the beginning of the treatment as cooling supports the resuscitation process in the sense that at lower temperatures, metabolic processes run slower, thereby supporting the replenishment of cellular substrate deficiencies.
Controlled Automated Reperfusion of the whole body.
CARL Therapy is a smart method of resuscitation after cardiac arrest. It was developed in an interdisciplinary collaboration between physicians and perfusionists at the Clinic for Cardiovascular Surgery at Freiburg University Hospital.
The new treatment method concerns sudden “acute cardiac arrest”, which until now can only be treated to a very limited extent even under optimal conditions. The survival rate in a hospital is about 20%. And, outside a hospital, only 3 to 8% of all patients survive an acute cardiovascular arrest. In addition, the few patients who leave the hospital often suffer from pronounced and persistent brain damage.
CARL Therapy relies on controlled restoration of blood flow through reperfusion. The former Medical Director of Cardiovascular Surgery at the Medical Center – University of Freiburg and his team of researchers have discovered that it is thus possible to resuscitate a person even after a prolonged cardiac arrest without significant consequential damage.

Statement Prof. Dr.-Ing. Benk
“To establish CARL Therapy in clinical practice, numerous innovative approaches in the field of medical technology were required. The visionary challenge was to be able to automatically control both the physical and biochemical perfusion conditions during extracorporeal circulation, both inside and outside the hospital.
We met this challenge – and today we have reached the point where our smart system can start its journey into hospitals.”
Prof. Dr.-Ing. Christoph Benk
Managing Director, Resuscitec GmbH

Statement Univ.-Prof. Dr. Dr. h. c. Beyersdorf
“After a cardiovascular arrest, the entire body is in a special state that must be understood very precisely and treated individually for each patient. Above all, the patient’s blood must be modified in such a way that the organs can gradually recover from the lack of oxygen supply. Based on the findings of our many years of clinical research, we have therefore developed a novel therapy for resuscitation, which we call CARL Therapy.”
Univ.-Prof. Dr. Dr. h. c. Friedhelm Beyersdorf
Founder and Initiator, Resuscitec GmbH
Former Medical Director of the Clinic of Cardiovascular Surgery at The Medical Center – University of Freiburg